Language and Health
As advocates for access to healthcare in a patient’s language of choice, our research focuses on the effects of linguistic or language-related factors in healthcare. This includes pioneering research on patient-provider language concordance in Canada, an important factor that has been found to affect care quality, patient outcomes, and healthcare expenditures.
FEATURED PROJECTS
Rethinking the Way We Measure Access to Language-Concordant Care
Traditional physician-to-population ratios overestimate Francophones’ access to French-speaking physicians (FSPs) by ignoring competition from non-Francophones. Using a competition-adjusted approach, this study found that Francophones are 8.8 times less likely to receive language-concordant care than Anglophones/Allophones. These findings have equity implications for healthcare planning and can be applied to other linguistic minority groups.
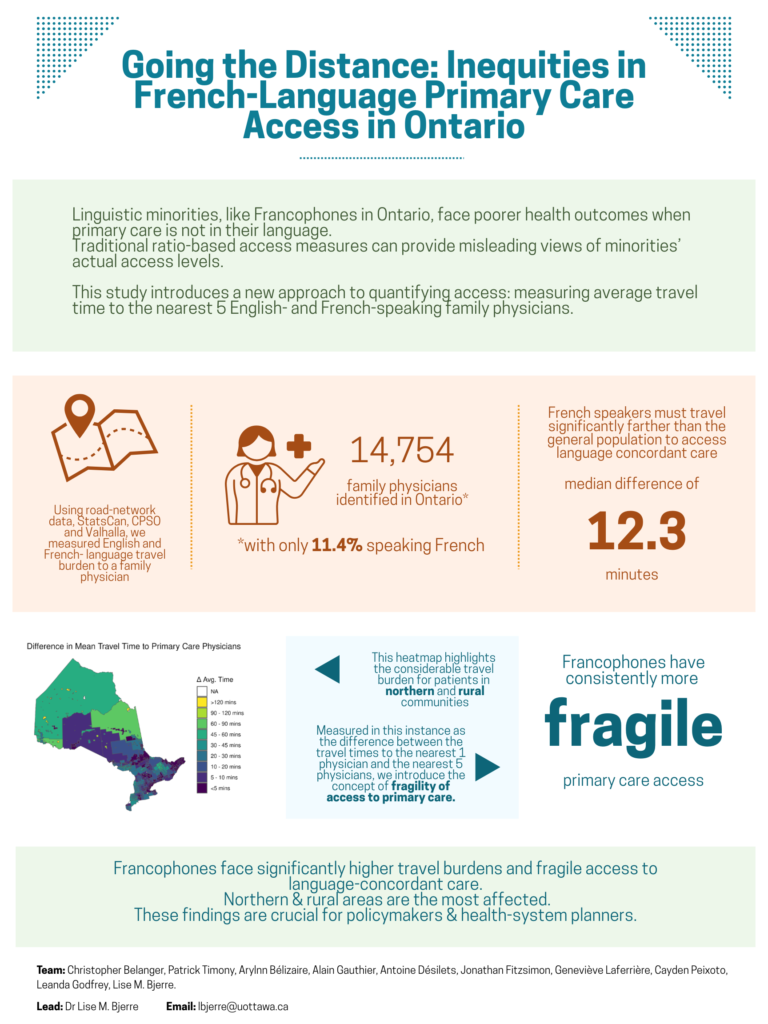
Measuring Inequities in Travel Burden and Primary Care Access Fragility
Francophones in Ontario face longer travel times and greater access fragility when seeking language-concordant primary care, particularly in rural and northern regions. This study introduces a new geospatial approach to measuring access, moving beyond traditional ratio-based methods. These findings highlight significant disparities and provide valuable insights for policymakers and health-system planners.
Geospatial Mapping to Determine Language Ability and Distribution of Family Physicians in Ontario
French-speaking family physicians in Ontario are unevenly distributed, with fewer providers per capita in rural and northern regions, where Francophones are more likely to live. This study maps these disparities, highlighting significant gaps in language-concordant primary care. More advanced access measures, such as travel burden analyses, are needed to fully understand and address these inequities.
Linguistic Factors and Inappropriate Prescribing in Long-Term Care
Francophones and other linguistic minorities in Ontario long-term care (LTC) homes face higher odds of potentially inappropriate antipsychotic prescribing (PIP-AP). Residents in language-discordant facilities were more likely to experience PIP-AP, highlighting how the linguistic environment can impact care quality. These findings emphasize the need for language-concordant care strategies in LTC settings.

Geospatial Analysis of Disparities in Access to Primary Care in Ottawa
French-only speakers in Ottawa face statistically significant but modest inequities in travel burden when accessing language-concordant primary care compared to the general population. These disparities are more pronounced in rural neighborhoods, where travel burdens are higher. The study’s findings can inform policymakers and serve as a model for assessing access inequities in other regions.